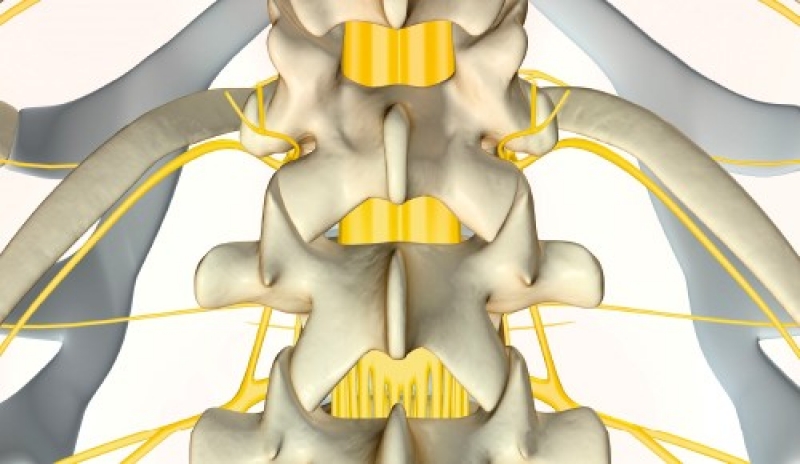
Cauda equina syndrome
This syndrome can be serious and can prompt legal claims if symptoms are misdiagnosed, say physios Laura Finucane, Chris Mercer and Sue Greenhalgh.
Cauda equina syndrome (CES) is a rare condition, occurring in one to three in every 100,000 people. Up to two people in every 100 with herniated lumbar discs may develop the condition. Without early interventions, the possible consequences can be devastating, including irreversible damage to bladder and bowel function, and sexual dysfunction.
Many patients seek help from a range of practitioners and delays in diagnosis can lead to long-term disabling consequences, resulting in costly negligence claims. The average cost of a CES claim is £336,000 (with about half this amount going to the patient). Delays are mainly caused by failures to recognise the signs and symptoms of the condition, delays in arranging MRI scans and delays in making referrals for surgical opinion.
For the best possible outcome, surgical decompression should take place as soon as practically possible, and within a few hours of the onset of symptoms. Current guidance tells us ‘nothing is to be gained by delaying surgery and much can be lost’ (Germon et al 2015).
CES occurs when the nerves below the spinal cord are compressed, with the most common cause being a prolapsed lumbar spine disc. Other conditions such as spinal stenosis and metastatic spinal cord compression can also cause CES.
There is no agreed definition of CES but the British Association of Spinal Surgeons’ definition is useful in clinical practice. This states: ‘A patient presenting with acute back pain and/or leg pain with a suggestion of a disturbance of their bladder or bowel function and/or saddle sensory disturbance should be suspected of having a CES.’
We know that most of these patients will not have a critical compression of the cauda equina (about 10 per cent of people showing the signs and symptoms of CES actually have the condition). Despite this, physiotherapists should have a low threshold for requesting further investigations, such as an emergency scan or making a referral to A&E.
Sue Greenhalgh (co-author of this article), James Selfe, from Manchester Metropolitan University, and Valerie Webster, from Glasgow Caledonian University, have worked with people with CES to develop a toolkit to aid clinicians and patients in the early identification of CES. The toolkit includes a cue card to help clinicians ask the right questions during the examination. The credit card for patients contains information of what to look out for and what to do if patients develop symptoms
Good communication is vital as patients with suspected CES may not see the relevance of the questions clinicians put to them, especially if they are experiencing severe pain.
Examination
Anyone suspected of having CES must undergo a detailed subjective and physical examination. The examination should include a full neurological assessment, including sensation of the perineum to light touch and pin prick along with a digital rectal examination to assess anal tone. These tests should be carried out only by clinicians with the appropriate training and competence.
Clinicians seeing patients with potential CES must have clear and robust pathways of care in place to enable rapid onward referral when appropriate. All staff should be aware of these pathways.
Laura Finucane, Chris Mercer and Sue Greenhalgh are consultant physios, at Sussex MSK Partnership, Western Sussex Hospitals NHS Trust and Bolton NHS Trust, respectively.
Source: http://www.csp.org.uk/frontline/article/clinical-update-cauda-equina-syndrome